Not that I ever left, but I am now back in the world of diabetes… You may have noticed that I have posted a little less over the past twelve months? Well, that’s because I have been completing a full time Masters in Dance Practices, teaching, performing, and managing online clients for Type 1 Active. Towards the end of the MA course, of which I achieved the final result of distinction, I became very stressed and let my diabetes management slip a bit. When I performed, the adrenaline hypers were difficult to control and when I was writing my dissertation I was sitting down a lot and not really taking the time to accurately count my carbs.
Not that I ever left, but I am now back in the world of diabetes… You may have noticed that I have posted a little less over the past twelve months? Well, that’s because I have been completing a full time Masters in Dance Practices, teaching, performing, and managing online clients for Type 1 Active. Towards the end of the MA course, of which I achieved the final result of distinction, I became very stressed and let my diabetes management slip a bit. When I performed, the adrenaline hypers were difficult to control and when I was writing my dissertation I was sitting down a lot and not really taking the time to accurately count my carbs.
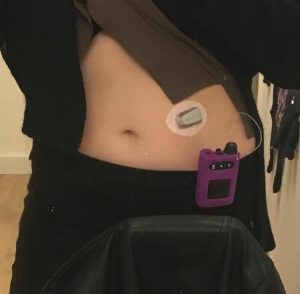
I know where I have been going wrong so it should be fairly straight forward to get myself back on track. In fact, things are looking up already because I connected to my CGM again and realised a few things that I already know. Like taking bolus at least twenty mins before I eat in order to avoid the spike. And ensuring basal doses throughout the day and night are correct.
A few of you have asked what I am up to, now that my studies have finished… I teach a lot of pole dance classes and one to one sessions, do online training for people living with diabetes, and I am just about to release a new product for Pole Purpose – it’s a creative resource pack for pole dancers. Alongside this I am reading for my PhD application. I would really love to delve deeper into my dance research so I am working really hard to make that happen over the next few months. Alongside all of the above I am keeping up with my own training and health maintenance.
My training pretty much involves, in no particular order, pole dance, contemporary dance, HIIT, cycling or walking, and yoga. I’m trying to keep the cardio at a lower intensity to give my body a break from all of the harsh pole / hiit training. I’m having one full day off a week, to regenerate both mentally and physically and it is helping a lot. I didn’t realise how shut off I’ve been from life with no day off.
Things you may have missed if you don’t follow me on youtube or Instagram,
Dealing with negative comments
My podcast interview with Rob Howe….
Two Very short trips to Paris and Las Vegas- pics on my insta.
Generally a lot of yoga and pole pics / videos…
Now that I have more time I will be vlog / blogging again so please let me know if there are any particular topics you want me to talk about.
Lots of healthy thoughts and happiness to you.
Rowena x
How do you like to eat when you travel? Do you work out whilst you are away? Let me know on Instagram, Twitter or YouTube.